Tuesday was a gorgeous day. I was working from home in the backyard under the patio umbrella. As my creative juices were flowing in front of my lap top I got a chill. More than a chill really, it felt like winter inside of my body. I chalked it up to sitting in the shade and threw on a sweatshirt. Finally I couldn’t take it and moved into the warm embrace of the sun. I let it soak into the fibers of my sweatshirt like a little oven. Eventually I just went inside and piled myself under blankets. A couple hours later I felt feverish so I took my temp. YUP…104 temperature. CRAP.
I knew what my fate was. I would have no choice but to check into Hotel de Women and Infants pretty much kicking and screaming.
Cory drove and stayed with me in the emergency room. Around 11pm I was admitted and moved to a room on the oncology floor. Prior to that they did a chest x-ray and drew more blood cultures. The end result is that I have another/still have the same (?) blood infection. I am neutropenic at the moment which means that I am low on white blood cells that would normally fight against bacteria and infection. This is common in cancer patients undergoing chemo. Our immune systems are just shot.
That said, if you are sick or even suspect you have a cold- GET THE HELL AWAY FROM ME.

This is currently on my hospital door with a box of super attractive bird flu masks
So I’m not going to dissect every detail of my time here so far because it’s exhausting. Here are the cliff notes:
- I will most definitely be here for a few days 😦
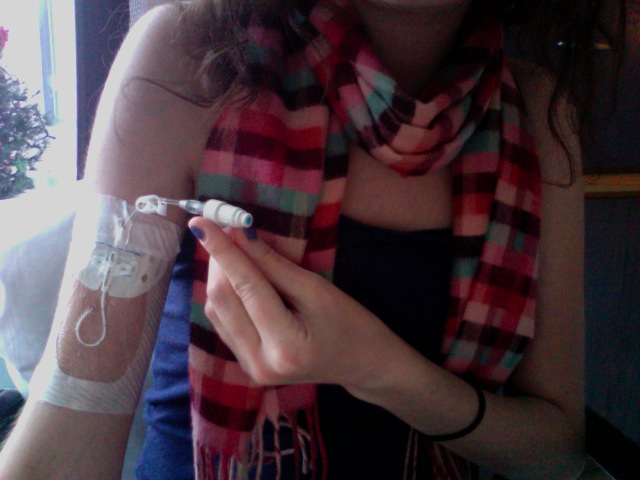
- My port just stopped working yesterday. Can’t flush it, can’t get a blood return. Nothing. That said I’ve had to have a couple peripheral lines put it (like normal IV’s) and that sucks a lot. I’ve had more needles jammed into me in the last 48 hours than I can count.
- Since my port was infected previously my doctors are erring on the side of caution and having it removed. It will happen sometime today but we’re at the mercy of whenever Rhode Island Hospital can do it so until then I must fast.
- They have two interventions to give me a boost and make me a little stronger. First it an injection to bump up my white blood cells. The other I am having as we speak and that is a blood transfusion. My hemoglobin was low so that should help too.
- Again, no port = tubes hanging from each arm uncomfortably. I’ve never missed my port more. I’m not afraid of needles but I certainly do not enjoy getting stuck with them multiple times a day.
With all this tubing hanging from my arms I’m tempted to recreate the fake party scene from Home Alone:
- No chemo this week so we can deal with the infection first
- Once the infection is gone they will be putting in a temporary PICC line (Peripherally Inserted Central Catheter). Eventually they will come out they will place a new port like the one I have now. Anyway, the PICC looks like this (photo cred: Happy Colon):
So those are the facts, here are the feels:
My initial reaction was anger. I’m actually still pretty angry which isn’t my typical response to something like this. I have just had so many hurdles thrown my way in such a short period of time, it’s exhausting. You are just always playing catch up to feel well. When will the day come that I can do that? If the last few months is any indicator it’s going to be an even longer road than I imagined.
I explained my frustration in these terms to a social worker on the floor. Most everything I do now has an asterisk next to it-
- I can go back to work but I can only be physically there 4 days a week
- I can take a shower but I have to spend 10 minutes taping a plastic bag over my port needle to keep it dry. (and DEFINITELY no swimming)
- I can go to that barbecue but I can’t eat any of the food there
You get the point, everything is conditional- at least for right now.
I get complimented often on my positive attitude which I sincerely appreciate. It’s still in there somewhere! I’m just salty at the moment. For now I need to honor and acknowledge the pain/anger/frustration because those feelings are authentic and part of the process.

Don’t worry George, it’s not the summer of Jess either.
Maybe there will be an autumn of Jess? Hope so.
































